History
What is Legionella?
In 1976, the United States of America celebrated the bicentennial of its independence from Great Britain and 200 years as a free and independent nation. In Philadelphia, some 4,000 members of the Pennsylvania State American Legion, or Legionnaires, an organization of World War II military veterans, gathered with their friends and families to attend the Legion’s 58th annual convention.
From 21 to 24 July, more than 600 legionaries were hostelled at the Bellevue-Stratford Hotel, considered one of the best accommodations in the city and, an important convention centre. But, ironically, instead of commemorating a great occasion and their brotherhood, the event would be remembered as one of the worst medical tragedies of the 20th century.
The day after the convention began, some Legionnaires began developing pneumonia-like symptoms: high fever, cough, chest pains and difficulty breathing. On July 27, an Air Force veteran who attended the convention, died in a hospital in Sayre, Pennsylvania, a few miles south of the New York State line. When the outbreak ended in mid-August, 221 individuals had contracted the as-yet-unknown disease and 34 of them had succumbed to the unknown illness.
An epidemiological study conducted by 20 medical detectives from the US Centres for Disease Control (CDC) was unable to effectively determine the cause of the outbreak, causing speculation to run rampant. There was a thought widely shared that the outbreak was caused by terrorists through chemical or microbiological means; others, that it was a failed CIA experiment; still others have suggested that the whole thing was a hoax, designed to encourage support for swine flu vaccinations. A Philadelphia toxicologist thought the outbreak was due to nickel carbonyl poisoning. Other speculations included toxic fumes from photocopiers and even an attack by extra-terrestrial forces.
After ruling a variety of medical illnesses, investigators found that the victims were staying in the same hotel, and suspicions were aroused.
After an exhaustive investigation of the source, spanning a number of months, it was discovered by the CDC that there was Legionella bacteria in the water supply of the hotel.
It wasn’t until December 1976 that Dr. Joseph McDade, a CDC lab scientist, using a guinea pig inoculation technique, was able to isolate the bacterium causing the disease and identify it as Legionella pneumophila. In April 1977, the term “Legionnaire’s Disease” was first published by the CDC as the official name of the epidemic disease. This caused Bellevue-Stratford Hotel to close permanently.
The dose of Legionella needed for infection is unknown, but it can be assumed that the infectious dose for susceptible humans is low, as patients are known to be infected after a few minutes’ exposure to the sources of some outbreaks and up to 3 , 2 km from the other source.
Infection depends on the level of water contamination by bacteria, the effectiveness of bacterial formation and spread through the air, host factors, and the virulence of the particular Legionella strain.
Legionellosis is an umbrella term that describes the pneumonic and non-pneumonic forms of Legionella infection.
The non-pulmonary form is an acute, self-limiting flu-like illness that usually lasts 2-5 days. The incubation period ranges from a few hours to 48 hours. The main symptoms are fever, chills, headache, malaise and muscle aches (myalgia). No deaths are associated with this type of infection.
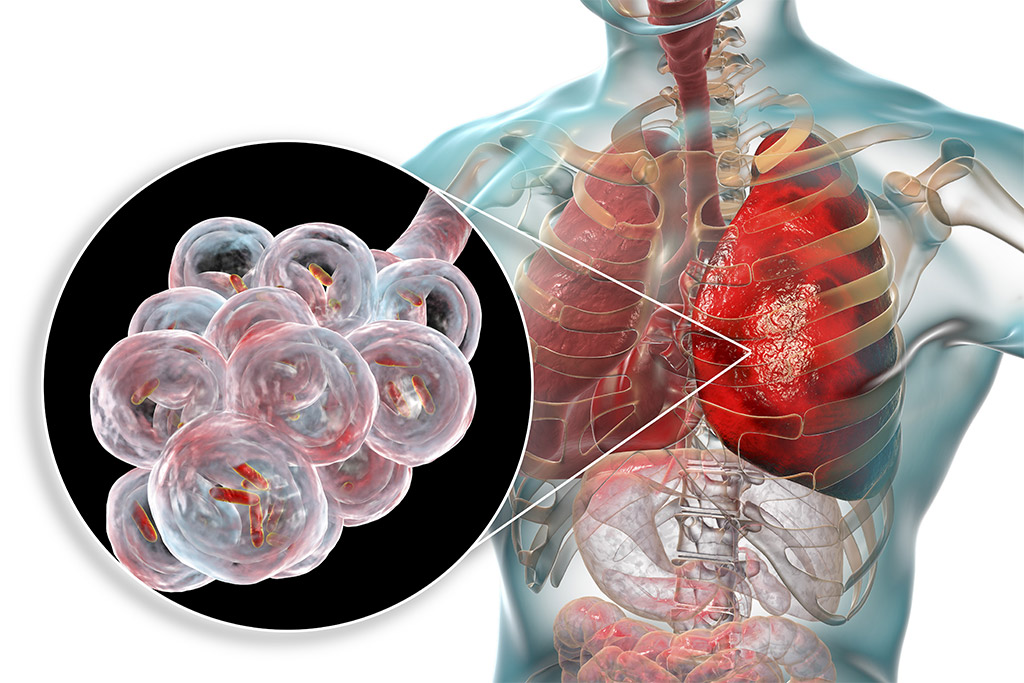
The pneumonic form, Legionnaires’ disease, has an incubation period of 2 to 10 days (but in some recent well-documented outbreaks, up to 16 days have been recorded). Initially, the symptoms are fever, loss of appetite, headache, malaise, and lethargy. Some patients may also have body aches, diarrhea and confusion. There is usually also a mild initial cough, but as many as 50% of patients may have phlegm. Blood-streaked phlemage or hemoptysis occurs in about one third of patients. The severity of the disease ranges from a mild cough to rapidly fatal pneumonia. Death occurs from progressive pneumonia with respiratory failure and / or shock and multi-organ failure.
Untreated Legionnaires’ disease usually worsens during the first week. In common with other risk factors that cause severe pneumonia, the most frequent complications of legionellosis are respiratory failure, shock, and acute and multi-organ renal failure. Recovery always requires antibiotic treatment and is usually complete after several weeks or months.
Mortality Rate
The death rate due to Legionella depends on: disease severity, appropriateness of initial antimicrobial treatment, context in which Legionella was acquired, and host factors (i.e. the disease is usually more severe in patients with immune suppression).
Case mortality rate can reach 40% -80% in untreated immunosuppressed patients and can be reduced to 5% -30% through appropriate case management and based on the severity of clinical signs and symptoms. For people who can develop an immune response, the mortality rate is usually between 10% and 15%.
The Cause
The causative agents, legionella, are freshwater bacteria found in aquatic environments around the world, but artificial water systems sometimes provide favorable environments for the growth of legionella bacteria. These bacteria survive within or between cells as parasites of living protozoa and within biofilms that develop in the water systems where the bacteria survive.
They can cause human infections by infecting other human cells using a similar mechanism to that used to infect protozoa.
Legionella. Pneumophila is the species most frequently isolated from patients with community-associated, travel-associated, or hospital legionellosis.
The installation of the AS SHOWER chrome is easy: simply replace the existing shower head with the AS SHOWER chrome. There is no need to change filter cartridges or carry out the periodic internal disinfection of the shower head – simply use the AS SHOWER chrome for the prescribed operating time and then replace it with a new one. Additionally, the AS SHOWER chrome can be used during thermal or chemical disinfection without affecting the filter performance.
 The genus Legionella includes Gram Negative bacilli, generally hydrophilic, which colonize natural aquatic environments (lake, river, springs, wetlands in general) and artificial (water networks of structures such as swimming pools, hotels, hospitals, houses, fountains, etc.)
The genus Legionella includes Gram Negative bacilli, generally hydrophilic, which colonize natural aquatic environments (lake, river, springs, wetlands in general) and artificial (water networks of structures such as swimming pools, hotels, hospitals, houses, fountains, etc.)
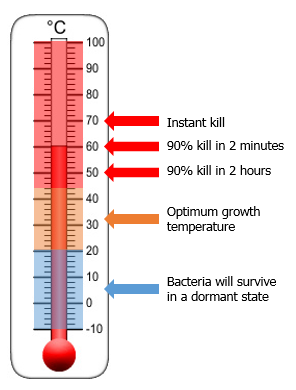
Legionella prefers habitats with warm water (preferably between 25° and 42° C but is able to survive in a temperature range between 6° and 63° C.
In water systems, legionella can be in free form, all ‘interior of ciliated protozoa (Tetrahymena) and potentially anchored to the biofilm (a film of microorganisms immersed in an organic matrix created in water networks especially after reduced water flow or long periods of inactivity).
Protozoa and biofilm represent a source of nourishment and protection from unfavourable environmental conditions (temperatures, biocides, etc.)
The formation of stable sessile communities is due to the activity of the “quorum sensing” (QS) regulation system, a communication system between bacteria capable of responding to the increase in population density.
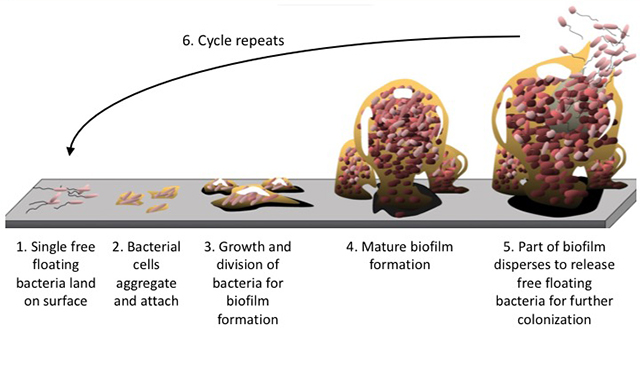
QS regulates the production of Acid Shock (ASP) or Heat Shock Protein (HSP) which allows microorganisms to counter and/or repair the damage caused by stress due to acid chemicals or temperature.
The most common form of transmission of Legionella is the inhalation of contaminated aerosols. Aerosol sources that have been linked to Legionella transmission include air conditioning cooling towers, hot and cold water systems, humidifiers, and whirlpools. Infection can also occur from aspiration of contaminated water or ice, particularly in hospitalised patients, and from exposure of children during water births. There is no direct human-to-human transmission.
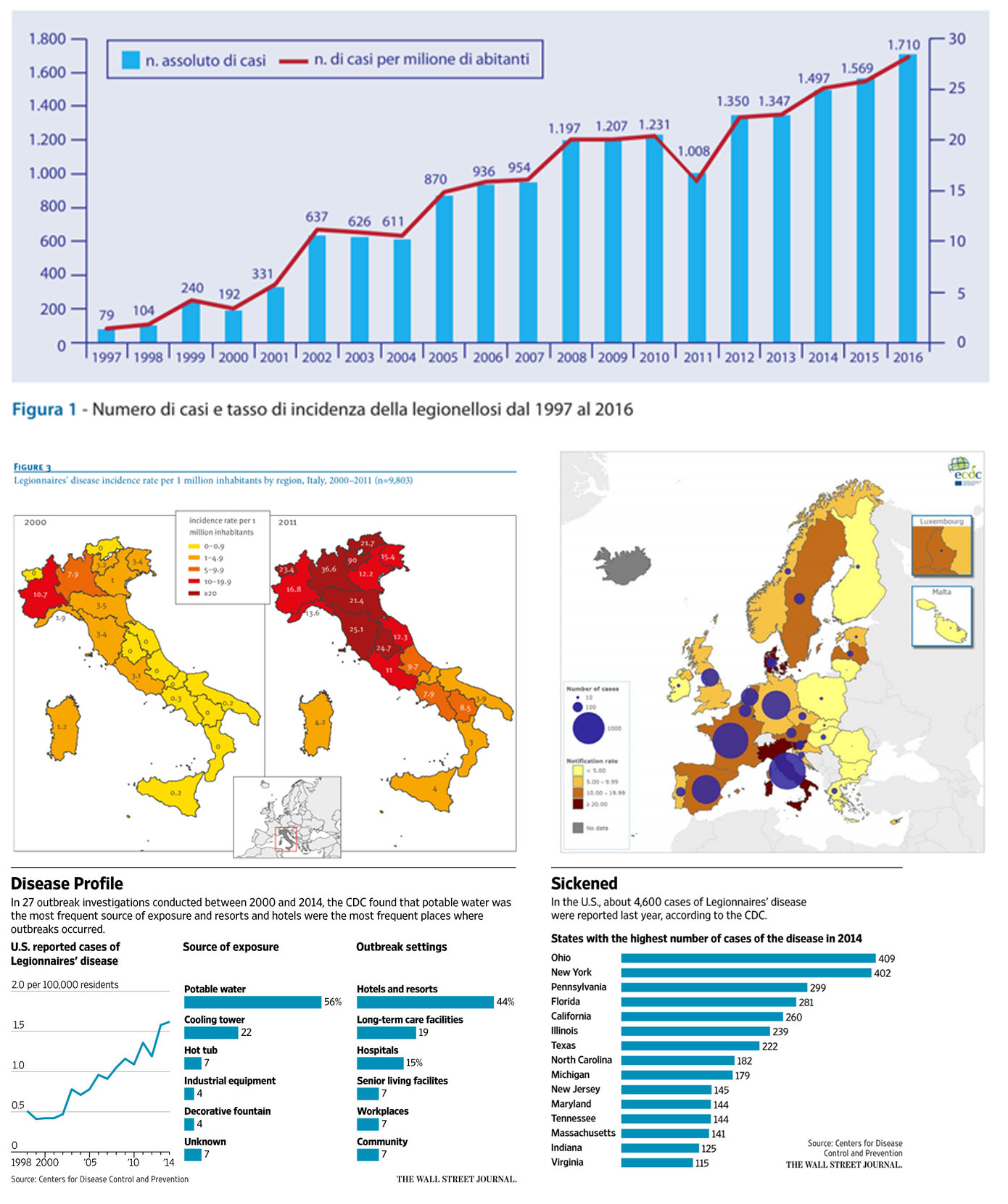
Legionella is present all over the world and finds its ideal habitat in technological systems. The registered cases are constantly increasing as well as the controls.